Share this
VP Activate™ - Our intelligent outreach solution
by Alex Bronk on July 1, 2023
Health systems are grappling with a myriad of challenges—from finances and patient health outcomes to rising consumer expectations and staff shortages. Health plans share similar challenges from consumers, especially as plan members continue to look for more from their health plans—including increased personalization, help with managing chronic conditions, and mental health support.
We all share the same concern regarding the lasting impact the last few years had on all of us—we’re struggling on both a physical level and a mental level. In their 2023 report, Mental Health America reports that 21% of adults (50 million Americans) are experiencing at least one mental illness, and over half (over 28 million individuals) receive no treatment.
With all these challenges, what are you to do? Consider enhancing your outreach and activation methods with a digital solution that offers a personalized experience.
In fact, 45% of providers think interventions—such as text reminders—have a positive impact on their patients’ ability to successfully follow their care plan for their chronic or complex conditions. 73% of patients would feel most inspired to take action on their health and wellbeing virtually (through a mobile app, by phone, via the web, or via video). Nearly half feel information and care they receive is too generic or not personalized.
Enhance your outreach and drive action
Meet VP Activate™, our intelligent outreach solution offering data-driven, health communications that stimulate action and deliver results.
VP Activate is a multi-channel, multi-cycle communication solution that drives acquisition, retention, and engagement through holistic and targeted outreach powered by advanced data modeling. With VP Activate, you can personalize motivation and impact receptivity via predictive modeling to better enable member action.
Our powerful technology supercharges your efforts
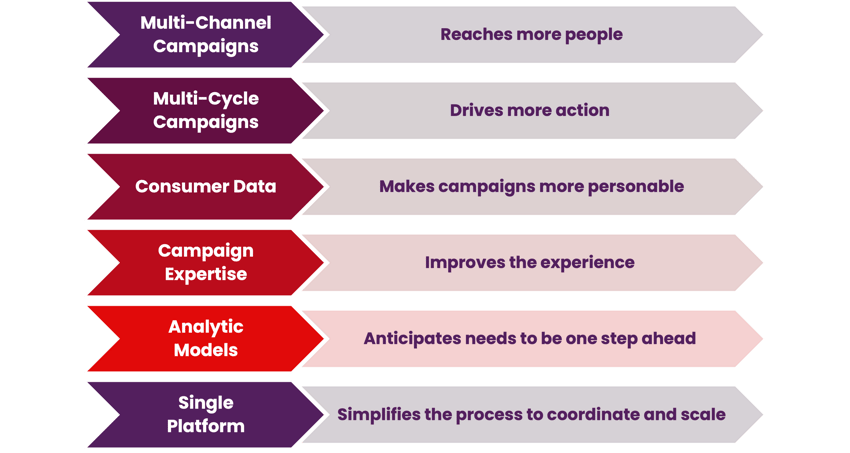
Health Plans: Improve your member experience and reduce risk

Regional plan closes diabetes gaps in care
Regional plan leverages personalized outreach and rewards to drive 20% of members to close all 3 diabetes gaps—which is important to their members' health, their plan’s quality measures, and Star Ratings.

Use multi-channel marketing to improve the member experience & reduce risk
Improve brand visibility and member satisfaction with the ability to reach ~90% of your population in the right marketing channel for each member.
Health Systems: Enhance your patient engagement and prospect acquisition strategy

Using the force of data to make a lasting impact
Health system embraces data and targeted campaigns to promote vaccine acceptance, acquire new movers, and send health risk assessment trigger campaigns to drive patient volume and earn high ROI.

How health systems acquire prospects & retain patients
Leverage our health system CRM and multi-channel marketing engine to reduce readmissions, promote screenings, manage chronic conditions, and drive high-margin services.
See it in action
Interested in learning more?
Contact your Strategic Account Executive and Account Management Team to get started.
Share this
- Employer (54)
- Program Tips (46)
- Wellbeing (40)
- International (29)
- Health Systems (23)
- Health Plans (18)
- Staying Healthy & Safe (15)
- VP Activate (15)
- Production Campaigns (12)
- Health (11)
- Webinars (11)
- Thrive Summit (10)
- Success Stories (7)
- Toolkits & Guides (4)
- Embracing Diversity (3)
- Mental health (1)
- May 2024 (1)
- April 2024 (1)
- March 2024 (2)
- February 2024 (1)
- January 2024 (5)
- December 2023 (2)
- November 2023 (1)
- October 2023 (2)
- September 2023 (4)
- August 2023 (5)
- July 2023 (4)
- June 2023 (2)
- May 2023 (1)
- April 2023 (4)
- March 2023 (1)
- February 2023 (1)
- January 2023 (1)
- December 2022 (2)
- November 2022 (7)
- October 2022 (6)
- September 2022 (2)
- August 2022 (4)
- June 2022 (2)
- May 2022 (5)
- March 2022 (1)
- January 2022 (1)
- December 2021 (1)
- November 2021 (1)
- October 2021 (2)
- September 2021 (2)
- August 2021 (1)
- July 2021 (1)
- June 2021 (3)
- April 2021 (6)
- March 2021 (1)
- February 2021 (3)
- January 2021 (3)
- December 2020 (2)
- November 2020 (2)
- October 2020 (2)
- September 2020 (3)